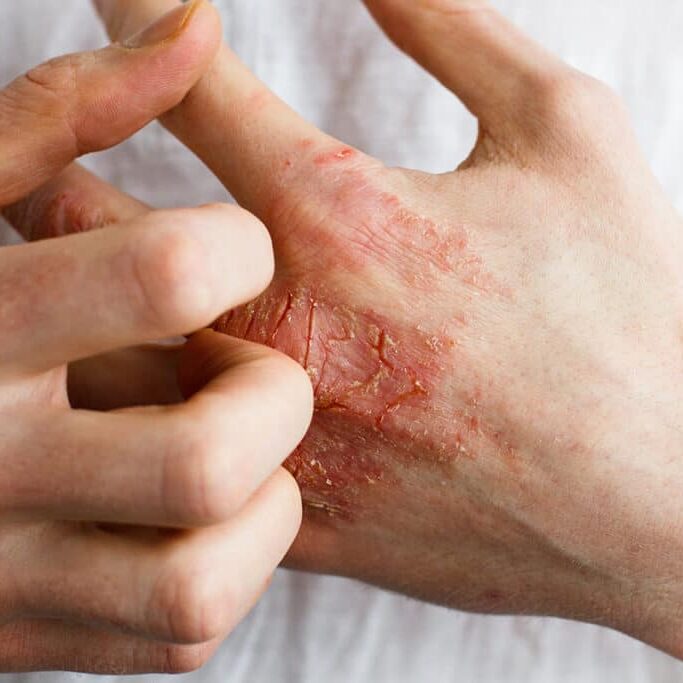
Unmasking the Mysteries of Seborrheic Dermatitis: Reclaiming a Flake-Free Scalp and Confidence
From Dandruff to Dermatitis
Understanding the Cause
A Journey Through Life
Beyond the Itch
Seborrheic dermatitis can be frustratingly itchy, and the associated flakes can be embarrassing. But remember, you're not alone! Effective treatment strategies are available to help:
Topical Antifungals
Corticosteroids
Ketoconazole Shampoo
Lifestyle Changes

Prevention is Key
Wash your hair regularly with a mild shampoo.
Avoid scratching your scalp.
Use a humidifier to add moisture to the air.
Manage stress levels.
Maintain a healthy diet.