How to Get Rid of Melasma: A Realistic Approach to Managing This Common Skin Condition
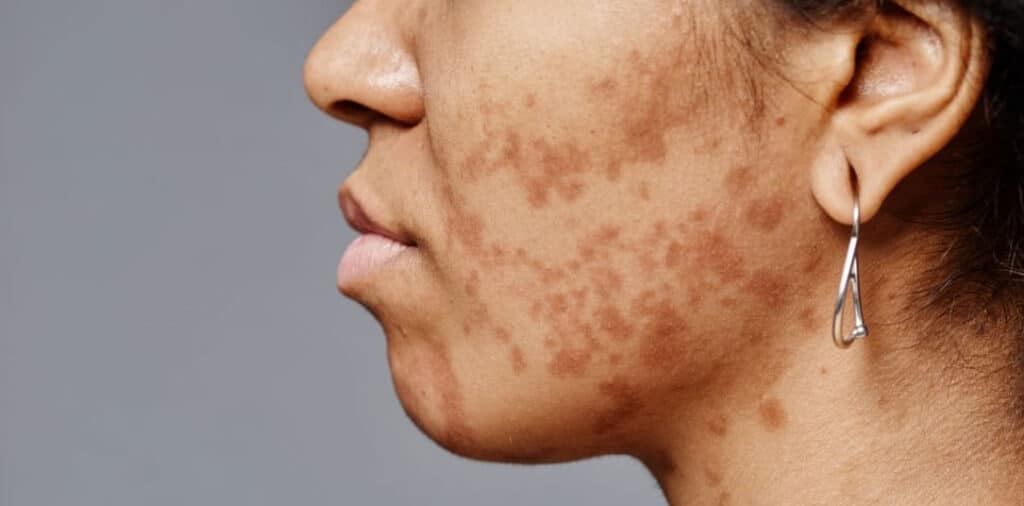
Those brown patches on your face that seem to appear out of nowhere and refuse to budge? You’re likely dealing with melasma, a frustrating skin condition that affects millions of people worldwide. If you’ve been searching for ways to get rid of melasma completely, this guide will provide you with the honest truth about this condition and effective strategies for managing it.
Melasma presents as patches of hyperpigmentation, typically appearing on the face in areas like the upper forehead, cheeks, and upper lip. These patches can range from light brown to dark brown, sometimes with gray or bluish undertones. The patches often have irregular borders and can vary significantly in size and intensity.
While melasma might feel like an insurmountable problem, understanding its nature and embracing realistic management strategies can help you regain control over your skin’s appearance. This comprehensive guide will walk you through everything you need to know about melasma, from its underlying causes to the most effective treatment approaches available.
Understanding Melasma: The Foundation of Effective Management
Melasma is fundamentally a hormone-induced condition that’s often hereditary. Unlike temporary skin issues that can be “cured,” melasma requires a different mindset altogether. The sooner you understand that melasma is a chronic condition requiring ongoing management rather than a one-time fix, the more successful your treatment journey will be.
Hormonal Factors Behind Melasma
Hormonal fluctuations serve as the primary trigger for melasma development. Pregnancy, often called “the mask of pregnancy” when melasma occurs, represents one of the most common triggers. The surge in estrogen and progesterone levels during pregnancy can stimulate melanin production, leading to those characteristic dark patches.
Birth control pills and hormone replacement therapy can also trigger melasma for the same reason. The hormones in these treatments can activate melanin-producing cells, causing them to create excess pigment in certain areas of the face.
The Genetic Component
If melasma runs in your family, you’re at a higher risk of developing it yourself. People with darker skin tones are also more susceptible to melasma, as their skin naturally produces more melanin. This genetic predisposition means that some individuals will always be more prone to melasma, regardless of their prevention efforts.
Sun Exposure as a Catalyst
While hormones may trigger melasma, sun exposure acts as a powerful catalyst that can worsen existing patches and stimulate new ones to form. UV radiation stimulates melanin production, which is why melasma patches often become more pronounced during summer months or after sun exposure.
Acceptance as Your Starting Point: Shifting Your Mindset
The most crucial step in managing melasma effectively involves accepting that this condition cannot be permanently “cured” in the traditional sense. This acceptance isn’t about giving up—it’s about redirecting your energy toward realistic, achievable goals.
When you accept that melasma is a manageable rather than curable condition, you can focus on strategies that actually work. Some people may experience complete clearance of their melasma over time, but this typically occurs due to natural hormonal changes rather than treatment-based interventions. For example, melasma that develops during pregnancy might fade after delivery as hormone levels normalize.
This mindset shift allows you to set realistic expectations and celebrate meaningful improvements rather than feeling frustrated by the condition’s persistent nature. Instead of asking “How can I get rid of melasma forever?” the question becomes “How can I best manage my melasma to minimize its appearance and prevent it from worsening?”
Comprehensive Management Strategies for Melasma
Sun Protection: Your Most Important Defense
Sun protection forms the cornerstone of any successful melasma management plan. Without adequate sun protection, even the most expensive treatments will fail to provide lasting results.
Daily sunscreen application is non-negotiable. Use a broad-spectrum sunscreen with SPF 30 or higher every single day, regardless of weather conditions. Look for sunscreens containing zinc oxide or titanium dioxide, as these physical blockers provide superior protection for melasma-prone skin.
Tinted sunscreens offer additional benefits for melasma management. These products often contain iron oxides, which help protect against visible light—a factor that can worsen melasma even when UV protection is adequate. Visible light from computer screens, indoor lighting, and reflected sunlight can stimulate melanin production, making tinted sunscreens particularly valuable for people with melasma.
Beyond sunscreen, implement comprehensive sun protection strategies. Seek shade during peak sun hours (10 AM to 4 PM), wear wide-brimmed hats, and consider UV-protective clothing for extended outdoor activities. Remember that sun exposure damage is cumulative, so consistent protection is essential.
Topical Treatments: Your Medical Arsenal
Several topical treatments can help lighten melasma patches and prevent new ones from forming. These treatments work by inhibiting melanin production or promoting cell turnover to reveal lighter skin underneath.
1. Hydroquinone: The Gold Standard
Hydroquinone remains the gold standard for melasma treatment. This bleaching agent works by inhibiting tyrosinase, an enzyme essential for melanin production. Available in concentrations ranging from 2% (over-the-counter) to 4% (prescription), hydroquinone can produce significant lightening effects when used consistently.
However, hydroquinone requires careful use. It can cause skin irritation, especially when first starting treatment. Some people may also develop a condition called ochronosis with prolonged use, which causes blue-black discoloration. Working with a dermatologist ensures safe and effective hydroquinone use.
2. Alternative Lightening Agents
Several other ingredients can help lighten hyperpigmentation when hydroquinone isn’t suitable or as part of a combination approach. Kojic acid, derived from mushrooms, inhibits melanin production and can be gentler than hydroquinone. Arbutin, a natural compound found in bearberry plants, offers similar benefits with minimal irritation risk.
Tranexamic acid, originally used to reduce bleeding, has shown promising results for melasma when applied topically. Licorice root extract contains glabridin, which can help lighten hyperpigmentation while providing anti-inflammatory benefits.
3. Retinoids for Enhanced Results
Retinoids, including tretinoin, adapalene, and tazarotene, can enhance melasma treatment by promoting cell turnover. When dead skin cells are shed more rapidly, pigmented cells are replaced by newer, lighter cells from deeper skin layers.
Retinoids also enhance the penetration of other lightening agents, making combination treatments more effective. However, retinoids can cause initial irritation and increase sun sensitivity, making gradual introduction and careful sun protection essential.
Chemical Peels: Accelerating Skin Renewal
Chemical peels can provide significant improvement for melasma by removing the top layers of pigmented skin and revealing lighter skin underneath. Different types of peels offer varying levels of intensity and results.
1. Superficial Peels
Glycolic acid and lactic acid peels represent the mildest option for melasma treatment. These alpha-hydroxy acids gently exfoliate the skin’s surface, promoting cell turnover without significant downtime. Multiple sessions are typically required for optimal results. Salicylic acid peels offer similar benefits with the added advantage of oil solubility, making them particularly beneficial for people with acne-prone skin alongside melasma.
2. Medium-Depth Peels
Trichloroacetic acid (TCA) peels penetrate deeper than superficial peels, potentially providing more dramatic results for stubborn melasma. However, these peels require careful post-treatment care and carry a higher risk of complications, including post-inflammatory hyperpigmentation.
3. Combination Peels
Many practitioners now use combination peels that incorporate multiple acids or add lightening agents to enhance results. These customized treatments can be tailored to your specific skin type and melasma characteristics.
Laser Therapy: Advanced Treatment Options
Laser therapy represents one of the most advanced options for melasma treatment, but it requires expertise and careful patient selection to avoid complications.
1. Pico Laser Technology
Pico lasers deliver ultra-short pulses of energy that can target melanin-producing cells without causing significant thermal damage to surrounding tissue. This technology can be effective for melasma, particularly when combined with other treatments.
2. Fractional Lasers
Fractional lasers create microscopic treatment zones while leaving surrounding skin intact. This approach can help lighten melasma while minimizing recovery time and complication risks.
3. Important Considerations
Laser treatment for melasma requires exceptional expertise, as improper technique can worsen the condition. The heat generated by some lasers can actually stimulate melanin production, leading to darker patches. Always seek treatment from experienced practitioners who specialize in treating melasma with laser technology.
Emerging Treatments: New Hope on the Horizon
Research continues to reveal new treatment options for melasma management. Platelet-rich plasma (PRP) therapy shows promise for some patients, using growth factors from your own blood to help reduce hyperpigmentation.
Exosome therapy, which utilizes cellular communication molecules, represents another emerging treatment that may help improve melasma by modulating cellular behavior and reducing pigmentation.
Tranexamic acid injections and oral supplements are also being studied as potential systemic treatments for melasma, offering hope for people who don’t respond well to topical treatments.
Essential Lifestyle Adjustments for Melasma Management
Beyond medical treatments, certain lifestyle modifications can significantly impact your melasma management success.
Hormonal Considerations
If you suspect that hormonal birth control is contributing to your melasma, discuss alternative contraceptive options with your healthcare provider. Non-hormonal methods like copper IUDs or barrier methods might help prevent melasma from worsening.
For women going through menopause, working with your doctor to find the lowest effective dose of hormone replacement therapy can help minimize melasma triggers while still addressing menopausal symptoms.
Skincare Routine Optimization
Establish a gentle, consistent skincare routine that supports your melasma treatments without causing irritation. Use mild, fragrance-free cleansers and moisturizers to maintain your skin barrier function.
Incorporate antioxidants like vitamin C into your morning routine to help protect against environmental damage and support your sun protection efforts. Apply vitamin C serum under your sunscreen for enhanced protection against both UV radiation and visible light.
Stress Management
While not directly linked to melasma, chronic stress can affect hormone levels and potentially influence the condition. Implementing stress management techniques like meditation, regular exercise, or yoga can support your overall skin health.
Dietary Considerations
Some people report improvements in their melasma with certain dietary changes, though scientific evidence is limited. Maintaining a balanced diet rich in antioxidants from fruits and vegetables supports overall skin health and may complement your treatment efforts.
Realistic Expectations and Long-Term Success
Successfully managing melasma requires patience and realistic expectations. Improvement typically occurs gradually over months rather than weeks, and maintenance therapy is usually necessary to sustain results.
Most people see initial improvement within 8-12 weeks of starting treatment, with continued enhancement over 6-12 months. However, individual responses vary significantly based on factors like skin type, melasma severity, and treatment compliance.
Remember that melasma can recur even after successful treatment, particularly with sun exposure, hormonal changes, or treatment discontinuation. This doesn’t represent treatment failure—it’s simply the nature of this chronic condition.
Building Your Personalized Melasma Management Plan
Creating an effective melasma management plan requires professional guidance tailored to your specific situation. A board-certified dermatologist can assess your melasma type, skin sensitivity, and lifestyle factors to develop the most appropriate treatment strategy.
Your plan might begin with topical treatments and sun protection, progressing to chemical peels or laser therapy if needed. Many people achieve excellent results with combination approaches that address melasma from multiple angles.
Regular follow-up appointments allow for treatment adjustments and monitoring for any side effects. This ongoing relationship with your dermatologist ensures that your management plan evolves with your needs and treatment response.
Moving Forward with Confidence
While you may not be able to permanently eliminate melasma, you can absolutely achieve significant improvement and maintain clearer, more even-toned skin with the right approach. The key lies in accepting melasma as a manageable condition and committing to evidence-based treatment strategies.
Remember that every person’s melasma journey is unique. What works for one individual may not be the best approach for another, which is why professional guidance and personalized treatment plans are so important.
By embracing realistic expectations, maintaining consistent sun protection, and working with qualified healthcare providers, you can take control of your melasma and achieve the clearer complexion you desire. The path forward may require patience and dedication, but the results—improved skin appearance and increased confidence—make the effort worthwhile.
Your melasma doesn’t define you, and with proper management, it doesn’t have to control your life. Take the first step today by consulting with a dermatologist who can help you develop a comprehensive plan tailored to your unique needs and goals.
Call today or book online to schedule your consultation at Smart Skin Dermatology in Lehi, Utah.

Lindsey is a board-certified Physician Assistant with over a decade of experience in dermatology. Born and raised in Salt Lake City, she earned her undergraduate degree in Human Movement Science from Utah State University on a full-ride soccer scholarship before completing her master’s in Physician Assistant Studies at A.T. Still University. She treats patients of all ages, with a special interest in acne, skincare, and cosmetic dermatology, and is passionate about education and helping train the next generation of physician assistants.