Eczema vs Psoriasis: How to Tell the Difference
Both eczema and psoriasis cause red, inflamed, itchy skin that can significantly affect your daily life. Yet these two common skin conditions require different treatments, and confusing one for the other often leads to frustration and delayed relief. Understanding the key differences between eczema and psoriasis helps you have a more informed conversation with your dermatologist and get on the path to proper treatment faster.
Quick answer: Eczema vs psoriasis
Eczema causes intensely itchy, dry, inflamed patches that typically appear in skin folds like the inner elbow and behind the knees, and it most commonly develops in childhood. Psoriasis produces thicker, well-defined, scaly plaques covered with silvery scales, usually appearing on the scalp, elbows, knees, and lower back, with onset typically between ages 15 and 35.
Eczema is fundamentally about a weakened skin barrier that allows irritants and allergens to trigger inflammation, and it’s often linked to allergies and asthma. Psoriasis is an autoimmune condition where the immune system drives skin cells to reproduce up to 10 times faster than normal, and it can be associated with psoriatic arthritis and cardiovascular disease risk.
Both are chronic, non-contagious, immune-related conditions that flare and improve over time. However, treatments effective for one condition may not work for the other. Only a dermatologist can reliably distinguish between the two through examination and, when needed, additional testing.
What is eczema?
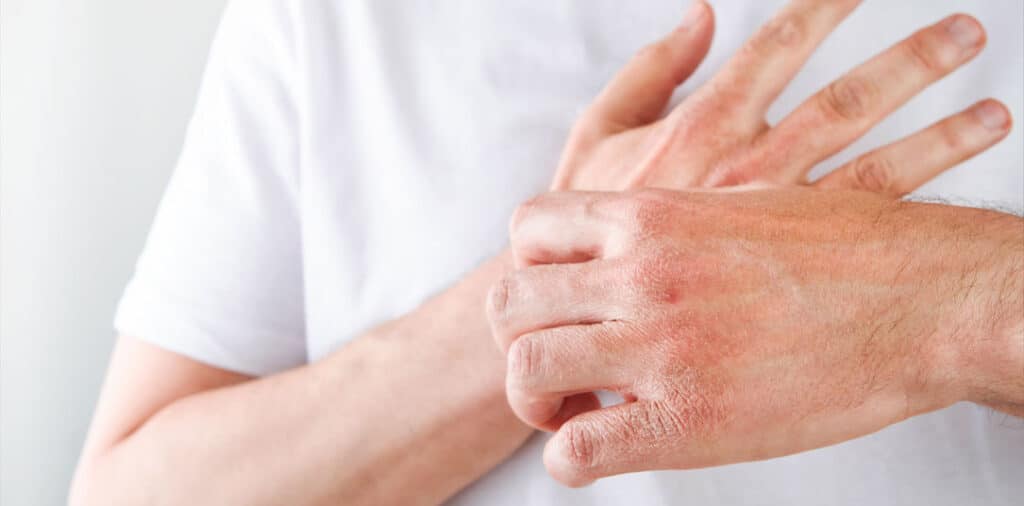
Eczema—most commonly atopic dermatitis—is a chronic inflammatory skin condition involving a weakened skin barrier and an overactive immune response to external triggers. When the skin barrier doesn’t function properly, irritants and allergens penetrate more easily, triggering an inflammatory cascade that produces the characteristic rash.
Eczema most often develops in infancy or early childhood, though it can persist into adulthood or even emerge later in life. Millions of Americans are affected, making it more prevalent than psoriasis in the general population.
The appearance varies by skin tone. On lighter skin, eczema typically looks red and inflamed. On medium-to-dark skin, patches may appear darker brown, purple, or gray. Regardless of skin tone, the affected areas are usually dry, rough, and may feel leathery over time.
The hallmark symptom is intense itching—often severe enough to disrupt sleep or cause bleeding from scratching. Eczema rashes tend to ooze or crust during flare ups and commonly affect flexural areas: inside the elbows, behind the knees, around the neck, and on the hands and face in older children and adults.
Eczema is part of what’s called the “atopic triad,” meaning it frequently occurs alongside asthma, hay fever, and allergies. A family history of these conditions increases the likelihood of developing eczema. This allergic association is one of the clearest ways eczema differs from psoriasis.
What is psoriasis?
Psoriasis is a chronic, immune-mediated disease where the body’s immune system becomes overactive and causes skin cells to grow at an accelerated rate. Normally, skin cells develop and shed over about a month. In psoriasis, this process takes only days, causing cells to pile up on the surface and form thick, raised patches.
Psoriasis typically first appears between ages 15 and 35, though a second peak occurs later in adulthood. While less common than eczema, psoriasis still affects millions worldwide and can range from mild patches to extensive coverage.
Plaque psoriasis is the most common form. On lighter skin, these plaques appear as raised, well-defined patches covered with thick white or silvery scales. On skin of color, plaques may look darker, violaceous, or gray, sometimes making diagnosis more challenging.
Unlike eczema, psoriasis tends to appear on outer surfaces: the scalp, outer elbows, front of the knees, and lower back. Nail changes—including pitting, ridging, and separation from the nail bed—are more characteristic of psoriasis than eczema. Joint involvement (psoriatic arthritis) affects a significant subset of psoriasis patients, causing pain and stiffness.
Psoriasis is fundamentally an autoimmune condition with systemic inflammation that extends beyond the skin. Research has linked it to increased risk of cardiovascular disease, metabolic syndrome, and related conditions—a systemic dimension that distinguishes it from the primarily skin-barrier dysfunction seen in eczema.
Eczema vs psoriasis: key differences
Although both conditions cause red patches and itching, several clinical features help distinguish eczema from psoriasis. The following comparison table summarizes the most important differences:
| Feature | Eczema (Atopic Dermatitis) | Psoriasis |
| Typical age of onset | Infancy or childhood | Adolescence to adulthood (15-35 years) |
| Itch quality | Very intense, often disrupts sleep | Milder itch with burning or stinging sensation |
| Rash borders | Ill-defined, gradual edges | Sharp, well-defined borders |
| Scale type | Fine or minimal, may ooze | Thick, silvery or white scale |
| Common locations | Skin folds (inner elbow, behind knees), face, hands | Scalp, outer elbows, knees, lower back |
| Associated conditions | Allergies, asthma, hay fever | Psoriatic arthritis, cardiovascular risk |
| Nail involvement | Rare | Common (pitting, ridging, separation) |
| Joint pain | Not typical | May indicate psoriatic disease |
At a glance, the most clinically useful differences:
- Eczema oozes during flares; psoriatic plaques typically do not—this is often described as the closest thing to a telltale sign
- Location matters: skin folds suggest eczema, while outer surfaces over joints suggest psoriasis
- Thick, silvery scales that flake off in sheets point toward psoriasis rather than eczema
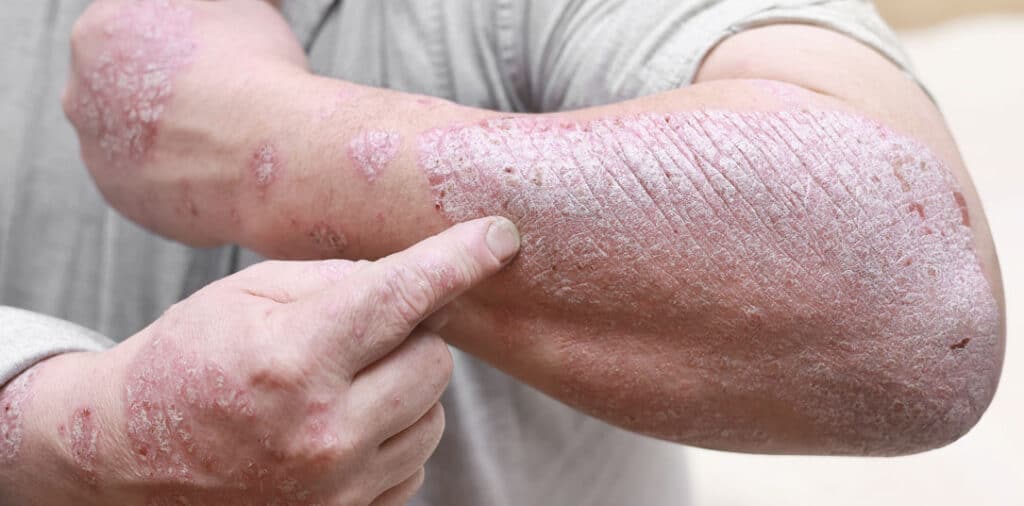
Differences in symptoms and appearance
How the rash looks and feels is often the first clue in telling eczema or psoriasis apart. While both cause inflamed patches, the quality of itching, texture, and appearance differ significantly.
Eczema symptoms include:
- Very intense itching that’s often worse at night, sometimes described as the most distressing symptom
- Dry, rough patches that may become leathery over time from chronic scratching
- Oozing, crusting, or weeping during active flares—a feature rarely seen in psoriasis
- Less sharply defined edges with a “patchy” or spread-out appearance
- Fluid filled blisters may develop in some forms like nummular eczema or contact dermatitis
Psoriasis symptoms include:
- Thick, raised plaques that feel bumpier and more solid than eczema patches
- Well defined borders with dense scale that can flake off in sheets
- Itching that may feel more like burning, soreness, or stabbing pain
- Nail changes such as pits, thickening, or white discoloration
- Joint pain or stiffness that might indicate psoriatic arthritis
Appearance also differs by skin tone for both conditions. On lighter skin, both typically appear red or pink. On medium-to-dark skin, eczema may look darker brown or gray, while psoriasis plaques can appear purple or violaceous. These variations can complicate self-diagnosis.
A concrete example: a child with weepy, irritated skin in the elbow folds who developed itchy patches early in life likely has eczema, while an adult with thick, silvery plaques on the outer elbows and scalp more likely has psoriasis.
Differences in causes and triggers
Both conditions involve the immune system but arise from different underlying mechanisms. Understanding these differences helps explain why the conditions respond to different treatments.
Eczema causes center on skin barrier dysfunction:
- A weakened or compromised skin barrier allows irritants and allergens to penetrate more easily
- Personal or family history of eczema, asthma, or allergies significantly increases risk
- Genetic and environmental factors both contribute, though the exact cause remains unknown
- The condition is inflammatory but not autoimmune—the immune system overreacts to external triggers rather than attacking the body’s own tissues
Psoriasis causes reflect an autoimmune process:
- T-cells in the immune system drive rapid skin cell turnover, creating the characteristic plaques
- Genetic susceptibility plays a major role, with family history of psoriasis or psoriatic arthritis increasing risk
- Systemic inflammation extends beyond the skin, which is why psoriasis links to conditions like cardiovascular disease
- The immune system is constantly overactive, not just responding to external irritants
Common eczema triggers include:
- Soaps, detergents, and skincare products
- Fragrances and certain fabrics (like wool)
- Hot or cold weather, dry air, and sweat
- Certain foods and seasonal allergies
- Emotional stress and managing stress poorly
- Skin infections
Common psoriasis triggers include:
- Throat infections (streptococcal infection can trigger guttate psoriasis)
- Certain medications like beta blockers or lithium
- Skin injuries (the Koebner phenomenon, where new plaques form at injury sites)
- Smoking and heavy alcohol use
- Obesity
- Stress
Identifying personal triggers is important for both conditions, but the typical trigger patterns and underlying pathways differ. Eczema flares respond to avoiding triggers and protecting the skin barrier, while psoriasis management focuses more on controlling the overactive immune response.
Differences in treatment approaches
Treatments for eczema and psoriasis overlap in some ways—both may benefit from topical anti-inflammatory creams—but long-term strategies differ because the underlying diseases are not the same. Proper treatment requires accurate diagnosis.
Eczema treatment (high-level overview):
- Daily, liberal use of moisturizers to repair and protect the skin barrier is foundational
- Short courses of topical corticosteroids help control flares
- Non-steroid anti-inflammatory creams provide alternatives for sensitive areas
- Severe eczema may require targeted prescription medications such as injectable medications or oral medications
- Trigger avoidance and gentle skincare routines help prevent flare ups
Psoriasis treatment (high-level overview):
- The goal is slowing rapid skin cell growth and reducing systemic inflammation
- Topical therapies work well for limited disease
- More extensive or resistant psoriasis may require light therapy (UV light or phototherapy)
- Systemic or biologic medications target specific immune pathways
- Joint involvement from psoriatic arthritis often changes the treatment plan significantly
For detailed information on specific treatment options, including medications and therapies, visit our dedicated eczema treatment and psoriasis treatment pages.
Both conditions benefit from:
- Trigger identification and management
- Gentle, fragrance-free skincare
- Regular follow-up with a dermatologist
- Lifestyle modifications including managing stress and avoiding known irritants
How doctors diagnose each condition
Dermatologists usually distinguish eczema from psoriasis through careful examination and questions about symptoms. Most cases don’t require special tests, but some situations call for additional evaluation.
During a typical clinical evaluation, your dermatologist will:
- Visually inspect rash patterns, noting thickness, color, borders, and type of scale
- Check common sites for each condition (scalp, elbows, knees versus skin folds, hands, face)
- Ask about age of onset and how symptoms developed
- Review family history of eczema, psoriasis, allergies, or asthma
- Inquire about joint pain, stiffness, or swelling
- Discuss potential triggers and what makes symptoms better or worse
In straightforward cases, diagnosis is based on appearance and history alone. The pattern of distribution, quality of scaling, and symptom characteristics usually provide enough information.
A skin biopsy may be needed when:
- The rash looks atypical or has overlapping features of both conditions
- Initial treatments haven’t worked as expected
- The affected areas are in locations where both conditions can look similar (palms, soles, genitals, scalp)
- Microscopic examination can reveal the rate of skin cell turnover and specific inflammatory patterns that confirm the diagnosis
Doctors may also screen for related issues. For eczema, this includes looking for skin infections or signs of barrier breakdown. For psoriasis, evaluation may include checking for nail changes, joint tenderness, and risk factors for cardiovascular disease or metabolic conditions.
The important takeaway: you don’t need to self-diagnose. Confusion between eczema and psoriasis is common even among experienced clinicians in certain body locations. Professional evaluation provides clarity.
Can you have both eczema and psoriasis?
Yes, it’s possible to have both eczema and psoriasis, though this is relatively uncommon. Some individuals have a strong genetic predisposition to inflammatory skin disease and may meet criteria for both diagnoses—either at different body sites or at different times in life.
In some patients, a single rash may have overlapping clinical features. Pathologists examining biopsy samples occasionally find mixed patterns, sometimes called “eczema-psoriasis overlap,” which complicates classification.
Why this matters:
- Treatments may need to be tailored carefully to address both conditions simultaneously
- Mislabeling one condition as the other can delay appropriate systemic therapy, particularly important if psoriatic arthritis is developing
- Some medications that help one condition may not adequately control the other
If your rash doesn’t fit classic descriptions of either eczema or psoriasis, or if you haven’t improved with standard treatment, seeking specialist evaluation makes sense. A dermatologist can determine whether you’re dealing with one condition, both, or something else entirely.
When to see a dermatologist
Persistent, very itchy, painful, or spreading rashes should be evaluated by a dermatologist rather than managed alone at home. Self-treatment with over-the-counter products has limits, and both eczema and psoriasis benefit from professional guidance.
Schedule an appointment if you have:
- A rash lasting more than a few weeks despite moisturizers and gentle care
- Severe itching that interferes with sleep, work, or school
- Thick, scaly patches on the scalp, elbows, knees, or nails
- Signs of infection including oozing, pus, yellow crust, or fever
- Joint pain, stiffness, or swelling along with a skin rash
- Uncertainty about whether your rash is eczema, psoriasis, seborrheic dermatitis, or another skin condition
Early diagnosis and personalized treatment can reduce flares, protect long-term skin health, and lower the risk of complications for both conditions. For psoriasis, this includes monitoring for psoriatic arthritis and cardiovascular risk. For eczema, it means preventing chronic skin changes and secondary infections.
If you’re unsure whether you have eczema or psoriasis—or if your current treatment isn’t providing relief—consider scheduling a comprehensive skin evaluation at Smart Skin Dermatology. Our dermatologists can provide a clear diagnosis, explain your options, and create a tailored care plan designed for your specific condition and skin type.

Carrie Jackman, PA-C, brings a unique blend of expertise, passion, and genuine care to Smart Skin Dermatology. Carrie’s passion extends beyond treating specific conditions. She thrives on building relationships with her patients, providing a warm and welcoming environment where everyone feels comfortable and heard. Her genuine care shines through in her interactions, ensuring each patient receives personalized attention and understanding.